A Physician Investigates: Should You Take Hydroxychloroquine?
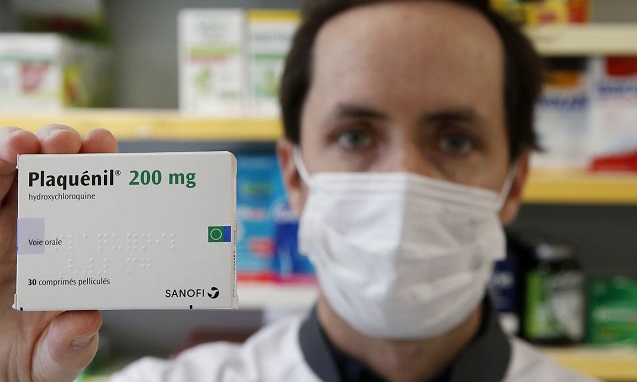
A controversy has arisen regarding the utility of using chloroquine or hydroxychloroquine with azithromycin in the prevention and treatment of COVID-19.
On the one hand, there are the purists who maintain that these medications ought not be employed until the proof of their benefits has been established. On the other, some advocate for the aggressive and immediate deployment of these medications. With these two very valid competing arguments proffered by sophisticated scientists and healthcare providers, the question for the rest of us mere mortals is what should we do?
The first step in addressing this question is to evaluate the state of the literature on the topic. An early indication that hydroxychloroquine or chloroquine in combination with azithromycin could be helpful in the treatment of CORVID-19 infection comes from a randomly controlled study from France involving 40 patients with early infection. All patients in the experimental group improved and did better than those in the placebo group, except for one who was 86 years old and received the medicines in an “advanced form” of the disease.
But the study suffered from its small size and lack of a peer review process.
Other studies seemed to support the French conclusion. In the laboratory, evidence demonstrates that chloroquine helps defeat the virus by increasing a cell’s internal pH and interfering with the penetration of the virus into the cell. Another study, this time out of China, showed the effectiveness of chloroquine and another medication, Remdesevir, against the SARS-CoV-2 virus (the COVID-19 virus) in Vero E6 cells taken from African green monkeys. Yet another preliminary study out of Wuhan showed that the time to clinical recovery, body temperature recovery time, and cough remission time were shorter in patients treated with hydroxychloroquine than in untreated controls.
There’s also experiential evidence suggesting that people who take chloroquine or hydroxychloroquine in low doses may be prevented from even developing the disease. Additionally, informally reported observations find that patients who regularly take these medications for other conditions such as lupus are generally not contracting COVID-19.
But conflicting scientific information has also emerged. One study suggests no benefit to the administration of hydroxychloroquine and azithromycin in patients with severe infection. The severe nature of the infections in these patients is notable, as it appears that the damage to the body goes beyond what an antibiotic can improve.
In light of all this emerging information regarding the potential benefits of administering the drugs it is tempting to conclude that we should treat all COVID-19 patients with these medications. But what about the potential harm? Here, there is extensive evidence of the safety of taking chloroquine and hydroxychloroquine. Yes, either medication can cause retinopathy and changes in heart electrophysiology, but these effects are exceedingly rare and take place in patients who consume the medication at higher doses and for much more protracted periods of time. In reality, the use of hydroxychloroquine or chloroquine in the recommended doses and projected administration times for COVID-19 is very safe.
So should we be taking chloroquine or hydroxychloroquine? Well, the answer actually comes in three packets.
- First, with the data available, those patients in respiratory failure ought definitely be treated with a regimen of chloroquine or hydroxychloroquine and azithromycin. They should also be placed on Remdesevir. These patients, of course, are generally being treated in the intensive care unit setting, and the optimal management controversy does not apply to the general public.
- Second, for those patients who are not in respiratory failure, but are nevertheless infected with COVID-19, the more proper approach is one of drug administration. Although treatment should be undertaken under physician supervision, there is little question that the balance between risk and benefit strongly lands in favor of benefit, especially when one considers the potential imminence of patient demise.
- Third, there is the question of preventive treatment or prophylaxis. Here again, there is a strong suggestion of benefit and a very remote risk of harm particularly when one considers the exceedingly low doses required for prevention. The conflict here lies in supply. Do we have enough chloroquine and hydroxychloroquine to meet the demands from such a broad swath of the population? Ideally, it would be preferable that everyone takes one of these medications, but in light of supply limitations, at the very least, those coming into frequent contact with COVID-19 patients and elderly persons should be on a prophylactic dose.
What about those on chronic regimens of these medications? Should they be kept from accessing chloroquine or hydroxychloroquine as many in the media claim is taking place? They shouldn’t. But even in light of temporary shortages, the prophylactic use of these medications should still be considered.
Let’s face it. We are looking at a massive pandemic that is devastating the national economy and able to take some victims with great haste. A short-term interruption of treatment on chronic patients is generally not going to result in their rapid demise, but the contraction of COVID-19 may. Here, urgency considerations definitely fall on the side of the COVID-19 patient and its prevention.
In the end, these are prescription medications so the decisions for administration or not lie with the physician. Ultimately, each physician is going to have to make up his or her mind. However, although there is still some room for debate, the answer presently is falling on the side of administering rather than withholding these potentially life-saving medicines.
© All rights reserved.
RELATED ARTICLES:
Crucial Facts About COVID-19: Transmissibility, Death Rates, and Raw Numbers